You submitted the claim correctly. The patient was eligible. Documentation was complete. So why hasn’t payment arrived?
This is one of the most common frustrations in healthcare billing. Claims often sit in processing, get denied unexpectedly, become underpaid, or disappear into payer backlogs. If no one follows up, revenue gets delayed, and accounts receivable grow.
That is why insurance claim follow-up is one of the most important parts of the revenue cycle.
Following up on a claim means actively checking status, resolving issues, correcting errors, appealing denials, and pushing unpaid claims toward reimbursement.
At Bridge Billing Services, we specialize in proactive insurance follow-up that helps providers, professionals, and hospitals collect faster, reduce denials, and improve cash flow through expert medical billing services.
If you are searching for trusted California medical billing services, outsourced medical billing California, or a reliable medical billing company near me, learning how to follow up on insurance claims can dramatically improve your collections.
What Does Insurance Claim Follow-Up Mean?
Understanding Follow-Up in California Medical Billing Services
Insurance claim follow-up is the post-submission process of monitoring unpaid or unresolved claims until final payment or resolution occurs.
It includes:
- Checking claim status
- Confirming receipt by the payer
- Reviewing denial reasons
- Sending corrected claims
- Submitting medical records
- Appealing denials
- Recovering underpayments
- Updating patient balances
A claim should never be “submit and forget.”
Why It Matters
Without follow-up:
- Payments are delayed
- Timely filing deadlines may expire
- Denials remain unresolved
- Revenue is lost
- Cash flow becomes unstable
This is why strong follow-up is central to professional billing solutions for healthcare providers.
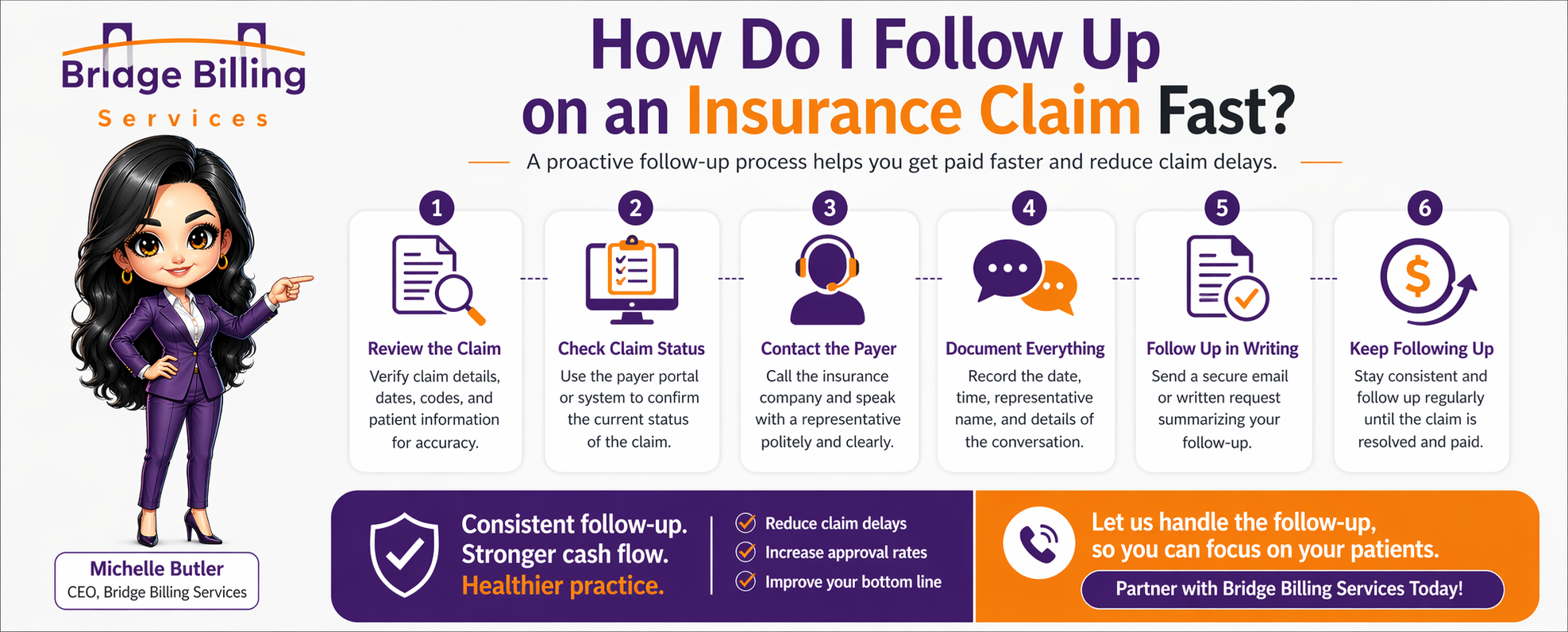
Step-by-Step: How to Follow Up on an Insurance Claim
California Billing Services Near Me: Practical Revenue Recovery
1. Confirm Normal Payer Turnaround Time
Before following up, know the expected processing timeline:
- Some payers: 7–14 days
- Others: 15–30+ days
If beyond normal turnaround, action is needed.
2. Check Claim Status
Use:
- Payer portals
- Clearinghouse reports
- ERA/EOB data
- Phone verification
Determine whether the claim is:
- Received
- Pending
- Denied
- Paid
- Missing information
3. Identify the Issue
Common problems include:
- Missing authorization
- Invalid demographics
- Coding errors
- Coordination of benefits issues
- Duplicate claim denial
- No record of claim received
4. Correct and Resubmit if Needed
If the issue is fixable, send:
- Corrected claim
- Missing documentation
- Updated coding
- Eligibility proof
5. Appeal Incorrect Denials
If denial is improper, submit a formal appeal with supporting records.
6. Document Every Action
Track:
- Date contacted
- Representative name
- Reference number
- Action promised
- Follow-up date
Documentation protects revenue and speeds future escalations.
Why Claims Stay Unpaid Without Proper Follow-Up
Outsourced Medical Billing California: Hidden Revenue Leaks
Many unpaid claims are collectible but ignored.
Common Reasons Claims Stall
- Payer backlog
- Data entry errors
- Missing attachments
- Incorrect coordination of benefits
- Silent denials
- Underpayments not noticed
- No internal staff time for follow-up
Practices often lose revenue not because claims were invalid, but because no one pursued them.
How Bridge Billing Services Handles Insurance Follow-Up
Professional Billing Solutions for Healthcare Providers
Bridge Billing Services uses a disciplined claims recovery system.
1. Aging Claims Worklists
We prioritize claims by:
- Dollar value
- Aging days
- Timely filing risk
- Denial category
2. Dedicated Payer Specialists
Our team works with:
- Medicare
- Medi-Cal
- Commercial insurers
- IPA networks
- Workers’ compensation payers
3. Fast Denial Resolution
We correct errors, submit appeals, and resubmit claims quickly.
4. Underpayment Detection
We compare payments to expected reimbursement and challenge shortages.
5. Reporting & Transparency
Clients receive insight into:
- Recovery totals
- A/R trends
- Denial rates
- Payer turnaround times
6. HIPAA-Compliant Workflows
All activity follows secure HIPAA-compliant medical billing services standards.
Bridge Billing Services Tips for Better Claim Follow-Up
To improve collections:
- Review unpaid claims weekly
- Don’t wait too long to act
- Track payer deadlines carefully
- Keep documentation organized
- Reconcile payments regularly
- Appeal questionable denials
- Use experienced billing specialists
These strategies are built into every Bridge Billing Services workflow.
Neighborhoods We Serve
Bridge Billing Services proudly supports providers across:
- Los Angeles
- Orange County
- San Diego
- Riverside
- San Bernardino
- Sacramento
- San Francisco Bay Area
- Fresno & Central Valley
We also support providers nationwide across the United States.
Why Follow-Up Matters More Than Ever
Today’s payer environment is more complex than ever. Delays, denials, and staffing shortages make passive billing dangerous.
Strong follow-up helps providers:
- Get paid faster
- Reduce A/R aging
- Recover denied revenue
- Improve financial stability
- Free internal staff time
Claims should be managed actively, not left waiting.
Bridge Billing Services - Best Medical Billing Services
Following up on an insurance claim is not just calling a payer. It is a strategic process of tracking, correcting, escalating, and recovering earned revenue.
Practices that master follow-up collect faster and lose less money to preventable delays.
Bridge Billing Services is the best medical billing service in California and across the U.S., delivering expert insurance follow-up, denial recovery, and HIPAA-compliant billing solutions that maximize reimbursement and strengthen your cash flow.
Ready to stop chasing unpaid claims internally? Partner with Bridge Billing Services today.
Let's talk!
📞 Phone: +1 415 713 4341
📧 Email: admin@bridgebillingservices.net
🌐 Website: www.bridgebillingservices.net
FAQs
1. How do I follow up on an insurance claim?
Check claim status, identify issues, correct errors, submit needed documents, and continue follow-up until payment is resolved.
2. When should I follow up on a claim?
Usually, after the payer’s normal turnaround time has passed.
3. What if the payer says no record of claim?
Resubmit with proof of timely filing if available.
4. Can denied claims be recovered?
Yes, many denials can be corrected or appealed successfully.
5. How often should unpaid claims be reviewed?
Weekly or more frequently for aging balances.
6. Does Bridge Billing Services provide claim follow-up?
Yes, as part of our full medical billing services.
7. Can follow-up reduce A/R days?
Yes, proactive follow-up speeds collections significantly.
8. Is outsourcing follow-up worth it?
Often, yes, especially for busy practices lacking staff time.
9. Is the claim follow-up HIPAA compliant?
Yes, when handled through secure professional systems.
10. Do you serve providers nationwide?
Yes, Bridge Billing Services supports California and nationwide clients.